Hands-off surgery
Sitting several feet from his patient, Sudhir Srivastava guides a robot through a single-vessel bypass.
By Amy Braverman Puma
Photography by Dan Dry
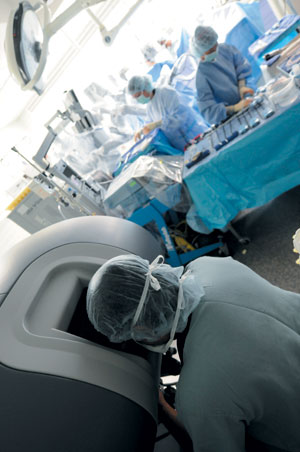
Wearing scrubs and a surgical mask, Sudhir Srivastava sits at a curved console, leaning forward to bury his head in a video screen. His hands grasp ergonomic controls under the monitor and his feet push pedals, all triggering four metal robotic arms positioned over a man lying eight feet away. The robot’s arms hold probes, inserted through 1–2–centimeter holes in the man’s torso, that mimic the movement of a human wrist.
It’s just past 9 a.m. in a University of Chicago Medical Center operating room. The patient, a 58-year-old, 241-pound man with a clogged coronary artery, was prepped at 5:30, anesthetized an hour later. On two monitors in the operating room, the surgical assistants, nurses, anesthesiologists, and visitors watch a tenfold magnification of what’s happening inside the patient’s chest. One arm uses a cautery to slit the patient’s reddish-orange, veiny chest wall, pulsing as the heart beats beneath it. Another wields microforceps—tiny tweezers with one-millimeter tips—to pull the wall apart. The cautery returns to scrape away yellow, jelly-like fat. At Srivastava’s commands, the robotic limbs, each holding their own tools, continue to peel layers apart until they reach their target, the left internal mammary artery.

Srivastava practices kriya yoga and meditation in his Kenwood home. The calming effects help him stay cool and focused during surgery.
“The speed will come, just like anything else, the more you do,” Srivastava says in a muffled voice, his face pressed to his own monitor, which not only magnifies the image but also shows it in three dimensions and high definition. He’s talking to a surgeon from Arkansas who’s come to observe the operation that Srivastava pioneered—a beating-heart, totally endoscopic coronary artery bypass (TECAB). Unlike traditional bypass surgery, during a TECAB Srivastava doesn’t cut open a patient’s chest but uses the robot to make those tiny holes—they’re smaller than most laparoscopic surgeries. Because he keeps the heart going, he doesn’t need a heart-lung bypass machine. And the robot’s agile arms and wrist-like movements provide “an even greater range of motion than the human hand,” the manufacturer says. It all adds up to less trauma to the body, fewer complications, less pain, less scarring, and only a week of recovery time and a bottle of Tylenol or aspirin.
Soon the OR observers see the shiny white mammary artery that is Srivastava’s target. Mammary arteries are more durable than the arm or leg veins grafted in traditional bypasses. And with the heart still beating, circulation remains intact, so it’s safe to put a mammary to a different use. “It’s interesting how close you can get without heat dissipation,” says E. J. Chauvin, the Arkansas surgeon, who’s thinking about bringing a robot to his own hospital. “The 3-D makes it very comfortable,” replies Srivastava.
The tools scrape the tissue and fat around the long white vessel, then finally cut the tube itself, leaving one end attached to the chest wall. Later Srivastava will graft the hanging strand to the patient’s clogged left anterior descending coronary artery to complete the bypass. “It absolutely requires a lot of patience,” Srivastava says. “Everybody will talk about how slow you are, but that’s OK.” In fact, he adds, “this part usually takes 20 to 30 minutes,” so it’s just as fast as open-heart surgery. The entire single bypass actually takes the same amount of time as the traditional route; although the procedure itself goes somewhat slower, Srivastava doesn’t have to spend time opening and repairing a patient’s chest. But a double, triple, or quadruple bypass can add a half-hour each to the operating time, so it takes a particular patience for a surgeon to keep his head in the console and to maneuver the robot to use the tiny instruments.
Fortunately Srivastava, unlike many surgeons known for their type-A personalities, has vast quantities of patience. He can sit at the console for hours unruffled. A Hindu from Jodhpur, a sunny tourist destination in India’s Rajasthan state, he practices kriya yoga and meditation, perfecting poses and breathing patterns every morning he can. He often does the exercises with his wife and, when they’re home, his son, 31, who lives in Seattle, and daughter, 27, in San Francisco. At age 60, Srivastava has been practicing yoga since he was a medical student in India in the late 1960s (he took a break from yoga this summer after having knee surgery; he was back at the robot’s console, however, after two-and-a-half weeks). “Yoga helps me to stay cool and persistent,” he says. “I’m just stubborn; you stay with it.”
Since 2003 Srivastava has performed 850 robotic heart surgeries—mostly bypasses but also valves, congenital defects, arrhythmias, lung resections. His long track record is what led Valluvan Jeevanandam, the Medical Center’s chief of cardiac and thoracic surgery, to recruit Srivastava, who joined the faculty in July 2007. Before that Srivastava had spent four years as the founding chairman of Odessa, Texas’s Alliance Hospital, where he perfected the robotic technique, practicing on pigs before operating on humans. Patients came from all over the country to go under Srivastava’s robotic knife, hoping to avoid having their chests cut open and the painful recovery.
Jeevanandam first met Srivastava in the mid-1990s, when they were both doing charity work at the same hospital in India. In 2002, four years after Jeevanandam joined Chicago’s faculty, the Medical Center bought its first da Vinci robot—the same year the machine was FDA approved. Made by Intuitive Surgical and named after the inventor of the first robot, it cost $1.6 million. Urological surgeon Arieh Shalhav pushed for the robot and continues to use it for prostatectomies. It’s also used in gynecological, transplant, vascular, and other coronary surgeries.
As the Medical Center’s cardio-thoracic section expanded its minimally invasive–surgery portfolio—implanting stents, heart valves, and other repairs using portals and robotic assistance—Jeevanandam began recruiting Srivastava, hoping to add bypass surgery to the list. It took two years to persuade him to come. “He owned the hospital, was a pillar of the community, was making double the money we could offer him here,” Jeevanandam says. “But there his data wasn’t validated. He needed to take it to an academic institution to legitimize the procedure.” Srivastava’s “vision,” Jeevanandam says, is to disseminate information about robotic heart surgery, to preach the gospel. And now that he’s here, Jeevanandam says, Chicago has “the most comprehensive minimal-invasive cardiac program in the world.”
The Medical Center bought a second da Vinci robot, mostly to accommodate Srivastava, who has dibs on it three days a week. Jeevanandam, who specializes in high-risk procedures including transplants, has only “dabbled” in robotic surgery. “My practice is people who are deemed too high-risk” for the method, he says. “It’s not the population that’s going to get robotic surgery.” And as cholesterol-lowering drugs and stents have made heart disease manageable without surgery, fewer low-risk patients were coming to Chicago, so Jeevanandam and Chicago’s other cardiac surgeons didn’t have much opportunity to practice using the robot. Srivastava brings not only years of experience but also his following of patients who find him on the Internet and travel the world to see him.
It’s also a matter of personality. Jeevanandam admits he doesn’t have the temperament for robotic surgery. For a simple task such as changing instruments using the da Vinci, “you have to stop what you’re doing, take one instrument out, put a new one in. Instead of taking a nanosecond it takes 30 seconds. Sometimes the camera lens fogs up and you have to take it out to clean it.” This past spring he was using a robot and “lost a plastic piece inside the chest,” he says. (“It wouldn’t have hurt the patient, but it’s better to be out rather than in.”) “It’s like finding a needle in a haystack. It took two hours to find it, and it was frustrating.” When hiccups like that occur, he often ditches the robot and switches to conventional open-heart surgery. “It takes a special personality,” he says, to keep with it rather than reverting to what he learned first, feeling with his own hands, to systematically solve a problem.
“We’re done with the mammary,” Srivastava says. It’s 9:20 a.m. An assistant stationed at the patient’s bedside manually pulls a robotic arm, the one holding the tiny camera, from the patient’s body and wipes the lens before reinserting it into the abdomen. Another assistant inserts another port, and the video screen shows the metal tube entering the man’s red insides. The new port squirts a clear liquid, papaverine, onto the mammary to dilate it.
While he waits for the artery to expand, Srivastava turns toward the heart, pulling away layers of tissue leading to the pericardium, the thin sac around the heart, which pulses beneath the membrane and more fat. He cuts a hole in the sac. “We’re going to expose the artery first,” he says, “so we’ll need a stabilizer.” Soon a clamp is holding part of the heart, keeping it still while the rest continues to beat.
The heart is surrounded by blood vessels, so maneuvering near it causes blood to squirt out, obstructing Srivastava’s view. A blower squirts water to wash it away. As he gets closer, he can see that the anterior artery is deeper inside the chest wall than expected. He’ll have to dig farther than he had anticipated.
More digging, more bleeding, more water squirting. It’s a regular part of the procedure, only more of it than usual. “He’s right on top of it,” says Chauvin. “It’s just deep.”
At 10 a.m. Srivastava pushes the pedal that focuses the camera, but the image stays fuzzy. “How come the camera is not focusing?”
One assistant suggests, “It’s probably you, sir.” But Srivastava still can’t focus. The operating room, where the assistants, nurses, and anesthesiologists have been quietly performing tasks or monitoring equipment, comes alive. The observers try to stay out of the way.
Another assistant: “CO2 is OK.”
They turn to the robotic arms. “Right coming in.”
“Left coming in.”
“Is a cable disconnected?” someone asks.
“No, because you would lose the picture totally,” someone else responds.
“Want us to reinsert the camera?”
“OK,” Srivastava says in a steady tone. “Reinsert the camera. All right, move fast.” As the assistants get on the job, he pulls away from the screen. “Get Mike,” he tells a nurse, referring to an Intuitive engineer.
Meanwhile the operating-room circulator, a kind of all-purpose nurse, fidgets with the robot’s base. He finds the camera’s manual focus and gets a clear image. He voices the remaining question: Why isn’t Srivastava’s pedal working?
The surgeon returns to the console. “OK, focus please.” The team will have to continue the operation using the manual focus, with either the nurse or Mark Dunkett, the Intuitive representative accompanying Chauvin, doing the honors. The surgical assistants slide the instruments back into the patient, and Srivastava returns to work with a clear image of the heart.
Such a malfunction is rare. In fact, Srivastava says later, it was the first time he had seen, let alone experienced, a camera-focus problem. “Things can happen with a machine,” he says.
But usually the machine cooperates—a good thing considering that cardio-thoracic surgery is hardly the only department that’s gone high-tech. The Medical Center has built up its offerings across the board. “What we’re doing in cardiac is an example where across the surgical programs we’re incorporating new technologies,” says Chair of Surgery Jeffrey Matthews. In urology, vascular, and cancer surgery, “we are at the leading edge of these technologies.” Chicago is one of the only centers in the Midwest, for example, to offer laparoscopic surgery for esophageal/gastric cancer and ulcerative colitis.
It’s especially important to remain top-notch in a city with five academic medical centers, “all vying for complex cases,” Matthews says—and the U of C, he adds, has the city’s lowest heart-surgery mortality rate. Cardiac surgery is particularly competitive because heart disease is the leading cause of death in the United States, because of the emerging technologies, and because insurance companies reimburse hospitals for much of the cost.
At a time when most hospitals are seeing a decrease in cardiac procedures, he says, staying stable would be good: at the University of Chicago the number is growing. In 2007 the Medical Center performed 524 cardiac surgeries; as of September 2008 the annual figure was already at 501. “If we’re going to stay at the forefront of medicine, we have to stay in front of the next big thing.” Among other additions to the cardiac team, Srivastava and his robotic expertise, Matthews says, were “a natural fit.”
At 10:30 a.m. Srivastava guides two of the robot’s arms, holding tweezers, to cut holes in the anterior artery. He threads a white, elastic string through the holes, where he’ll attach the other end of the mammary. He tightens the string to stop blood from flowing through.
By now the mammary has dilated—it’s big and shines blueish-silver. “It looks nice,” says Chauvin. Srivastava uses the tweezers to shimmy the string toward the mammary, then threads about ten U-clips through the side of the vessel, one at a time. He’s almost done sewing the arteries together when a machine starts beeping loudly. “Nonrecoverable fault,” reads the monitor. The computer needs to reboot. It’s another rare mechanical problem.
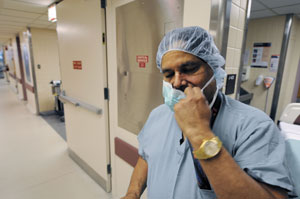
After a long surgery Srivastava leaves the operating room and removes his surgical mask. "It worked out OK," he says.
The assistants restart the machine, and Srivastava returns to sewing. Around 11:20 an observer asks if the surgery is taking longer than usual. “Normally we’d be done by now,” he says. The time killers—the camera focus, the deeper-than-normal artery, the reboot—haven’t broken his composure.
By 11:45 he’s finished with the bypass. A technician brings out an ultrasound to test the blood flow. She reads off some numbers. Pleased with the report, Srivastava lays the globs of fat and layers of tissue back over the heart. “All right,” he says. “Thank you all.” The lights, which had been dimmed, switch back to full fluorescence. Machines get unplugged and wheeled away.
Srivastava leaves the operating room and removes his surgical mask. “It worked out OK,” he says. “There was good flow through the bypass, and ultimately that’s what’s most important.”
Addressing Chauvin, he notes that when glitches occur, “it’s so easy to give up and convert” to traditional surgery. “Everyone has a different tolerance with it.” Chauvin responds, “And the patient was stable the whole time.” None of the holdups affected the man, who was discharged four days later. The procedure impressed the Arkansas surgeon enough that the Conway Regional Medical Center purchased a da Vinci machine and began its own robotic heart-surgery program in September.
Srivastava heads up to his fifth-floor office for a brief break and e-mail check. He and the robot must repair another heart this afternoon.

The da Vinci mode
Technically, it’s robot-assisted surgery. The da Vinci robot, approved by the FDA in 2000, “cannot be programmed, nor can it make decisions on its own to move in any way or perform any type of surgical maneuver,” assures Sunnyvale, California–based maker Intuitive Surgical on its Web site. In other words, rather than attempting to make surgeons obsolete, the robot relies on expert surgeons and aims to make them better.
Sitting at a video-game–like console, before a three-dimensional, tenfold image of the operating field, an expert like University of Chicago cardiac surgeon Sudhir Srivastava uses all four limbs—his hands holding controls, his feet pushing pedals—to guide the robot’s four arms, which surgical assistants, stationed at the patient’s bedside, insert through dime-sized holes into the patient. Attached to the arms are probes that Intuitive calls EndoWrist Instruments, modeled after the human wrist. The probes, one holding a tiny camera and the others surgical tools, “offer an even greater range of motion than the human hand,” and they can relay “force-feedback sensations” back to the surgeon, a substitute for tactile sensation. And a robot’s hand is steadier than the coolest of yoga masters.
By this past March Intuitive had sold 867 da Vinci units worldwide, 647 in the United States. And Srivastava isn’t the only University of Chicago surgeon to use the Medical Center’s two robots. Urological surgeon Arieh Shalhav pushed to bring the first one to Chicago in 2002; he and colleague Gregory Zagaja remove cancerous prostates with it. Vascular surgeon Hisham Bassiouny repairs abdominal aortic aneurisms. Gynecological oncologist Sarah Temkin performs hysterectomies to treat endometrial cancer. And other cardiac surgeons use the robot, including Jai Raman, who specializes in complicated cases.
An emerging technology for most of the world, the robot at Chicago has become fairly routine. And Srivastava, with 850 robotic surgeries behind him, including more than 300 bypasses, is the world’s leading robotic-bypass surgeon. “This surgery is not experimental in our hands,” he told the Biological Sciences Division magazine, Medicine on the Midway. “We’ve perfected our technique.”—A.B.P.
Return to topWRITE THE EDITOR
DISCUSS THIS ARTICLE
EMAIL THIS ARTICLE
SHARE THIS ARTICLE
MORE FROM THE MAGAZINE
RELATED LINKS
- Sudhir Srivastava’s Medical Center Web page
- Heart surgery at the Medical Center
- Intuitive Surgical’s da Vinci robot

