|
||
      |
Next Generation
Flight time
Physicists aren’t the only ones interested in determining the location and velocity of subatomic particles. That same information allows physicians, for instance, to make earlier and more precise cancer diagnoses. “The electronics needs in medical imaging,” says Chicago physicist Henry Frisch, “look very closely related to the needs we have in high-energy physics.”
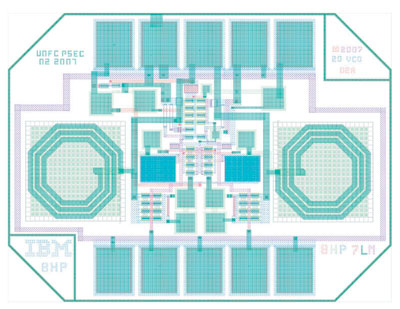
Specifically, Frisch, with Chicago radiologist Chin-Tu Chen, PhD’86, and Argonne physicist Karen Byrum, is working to build microchips—like the one below, which measures 850 microns across—that would improve the speed and accuracy of “time-of-flight” PET scans, a technique offering more precise images of vital functions such as glucose metabolism, blood flow, and oxygen use.
Conventional PET scans work by detecting the energy released after a short-lived radioactive isotope is injected into the body and absorbed into the organs. The isotope decays, giving off positrons that collide with neighboring electrons, a process that generates millions of photons—including numerous spurious signals that require intense computational analysis to filter out before the data is converted into images.
Time-of-flight PET scans, meanwhile, not only detect photons as they travel in opposite directions, but also measure the time difference between them, a calculation that helps construct clearer pictures and weed out false signals.