An Apple a day
Untethered from computers, Medical Center residents reconnect with patients using iPads.
By Burke Frank, ’11
Photography by Dan Dry
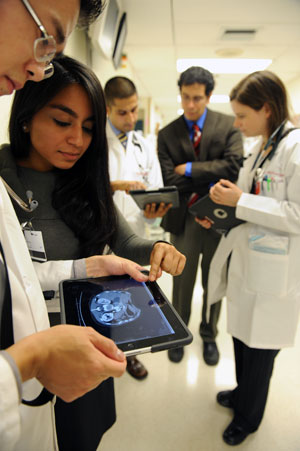
Symptom: Medical Center residents were spending too much time with computers and not enough with patients.
Prescription: iPads
Although modern medical technology offers doctors greater insight into patients’ insides, it often forces physicians to spend more time with their screens than in the wards. The best learning experience for residents remains at the bedside, says James Woodruff, director of internal-medicine residency at the University of Chicago Medical Center, but electronic records, test results, and massive reference resources have physicians “fighting for access” to limited computer space.
To address the problem, the residency program has turned to a sleek, handheld piece of hardware to put doctors back in touch with patients—the iPad. In November the Medical Center distributed 115 iPads to its internal-medicine residents. An Apple representative said it believed the Medical Center was the first in the country, and probably in the world, to use the devices on such a scale in its residency program.
With an iPad, doctors can access electronic resources at a patient’s bedside. If a CT scan finds a mass in a patient’s lung, Woodruff says, “the physician could open up a high-resolution image and put it in the patient’s lap so that the patient could actually see their study, see the lung nodule, and better appreciate the recommendations being made by the physician.”
Bhakti Patel, a chief resident at the Medical Center, agrees that quickly sharing information has benefits. Showing an X-ray that reveals a fracture or a tumor gives patients a sense of control over their treatment. “They feel a lot more empowered,” Patel says. “It makes them feel like they’re part of the treatment team and have a better understanding of what’s going on.”
But the greatest improvement, according to Woodruff, has been residents’ increased efficiency: “In the best of circumstances it saves hours to their day.” The streamlining pays off at the end of a resident’s call cycle, says Patel. The residency program accrediting council limits residents to 24 consecutive hours of “continuous duty time,” on-call and scheduled clinical hours, followed by a six-hour period to wrap up their work. Any care left unfinished at the end of 30 hours is passed on to another resident. If a physician is working with a complicated case, the pressure builds to finish quickly to limit interruption as the case gets passed to a new doctor.
With the new technology, glitches inevitably occur. The iPads are expensive and sensitive, making them potential targets of theft and tampering. The hospital invests about $650 in each iPad, including insurance, protective covers, straps, and applications, according to Woodruff. Required applications on each resident’s iPad include the New England Journal of Medicine for reference, Citrix for access to records, and MedCalc, which provides medical calculations and formulas.
To keep patients’ personal information safe, the devices are password protected and do not store records, Woodruff says: they serve as a portal for access through the hospital’s wireless network.
As with any hospital device, the iPads are a potential source of infection. All equipment larger than a cell phone undergoes frequent and intense cleaning with harsh disinfectants, Woodruff says, but the iPad’s sensitive screen would not withstand the agents. A special cover keeps it clean and safe from chemicals.
For advice on how to use the iPad in a major research hospital during the three-month pilot program, one resident “e-mailed [Apple CEO] Steve Jobs personally to ask him about his thoughts,” Patel says, “and he actually replied to her e-mail.”
That contact led to a high-level meeting within hours. “The head of medical applications for Apple was in communication with our resident,” Woodruff says, “and by the next morning we had a meeting with Apple leadership in our cafeteria.”
Although there are no plans to expand the iPad program to Medical Center physicians and faculty, Woodruff says, some have expressed interest in using them. “It’s another example of how technology can help facilitate care,” Patel says. “What this technology has done has turned our residents back to where the learning is happening, which is with the patient.”
Return to top
